Epidemiology of Mumps Infection
B. Epidemiology
Mumps is a disease of childhood, the highest incidence occurs
in children between 5 - 9 years of age. The disease is less
contagious than other childhood diseases such as measles and
varicella. According to a recent epidemiological survey in
America, 10% of the population had mumps during each of the first
5 years of life, 74% had it by age 10, and 95% by 20 years of
age. Mumps is endemic in most urban areas. In temperate zones, a
seasonal variation is evident, the highest incidence being around
January to May. No such seasonal variation exists in tropical
countries. Subclinical infections are common in very young
infants (2 - 3 years of age), and the proportion increases with
age in adulthood. Up to 90% of infections at the age of 10 - 14
age were associated with symptoms whilst almost all infections
are subclinical beyond 60 years of age.
C. Pathogenesis
Mumps is transmitted by droplet spread or by direct contact.
The primary site of viral replication of the epithelium of the
upper respiratory or the GI tract or eye. The virus quickly
spreads to the local lymphoid tissue and a primary viraemia
ensues, whereby the virus spreads to distant sites in the body.
The parotid gland is usually involved but so may the CNS, testis
or epididymis, pancreas and ovary. A few days after the onset of
illness, virus can again be isolated from the blood, indicating
that virus multiplication in target organs leads to a secondary
viraemia Parotitis is the most frequent presentation, occurring
in 95% of those with clinical symptoms. Occasionally, meningitis
may precede parotitis by a week. Virus is excreted in the urine
in infectious form during the 2 weeks following the onset of
clinical illness. It is not known whether virus actually
multiplies in renal tissues or whether the virus is of
haematogenous origin. Life-long immunity is the rule after
natural infection, but reinfections can occur and 1 - 2% of all
cases are thought to be reinfections.
D. Clinical_Features
The incubation period is 16 - 18 days but may vary from 14 - 25 days. Parotid swelling develops in 95% of those with clinical illness. The rate of subclinical infection varies with age, but is on average 30%. In a small proportion of patients, the symptoms may resemble mild URTI. Typically, a prodromal illness consisting of headache, malaise, myalgia and low grade fever occurs 1 - 2 days before the onset of parotid enlargement. Patients with classic mumps develop enlargement of one parotid gland, followed 1 - 5 days later by enlargement of the contralateral gland. The patient complains of pain and tenderness in the area of the gland. The submandibular and sublingual glands may occasionally be involved. The parotid swelling starts to subside after 4 to 7 days. Virus shedding into the saliva begins a couple of days before the onset of parotitis and ends 7 to 8 days later.
Complications
All the other manifestations of mumps can be regarded as systemic complications of mumps rather than as true complications.
E. Laboratory Diagnosis
During mumps infection, several non-specific findings may be present in the blood. The WBC may be low with lymphocytes predominating. ESR and CRP may be normal or slightly elevated. Amylase levels may be elevated.
1. Serology ;- a serological diagnosis is usually made by finding a significant increase in Ab titres in 2 serum samples taken 10 - 14 days apart. In some cases, the detection of IgM may be used to diagnosis acute infection. Although only 1 serotype of mumps exist, cross-reactions between mumps virus and paramyxovirus makes serological results difficult to interpret on occasions. Several techniques are available :
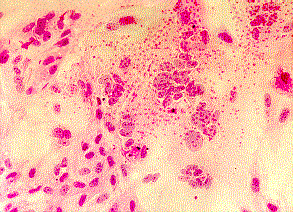
2. Virus Isolation ;- virus isolation may be carried out by allantoic inoculation of 6 day old embryonated eggs or by tissue culture methods. Virus can be isolated from the CSF during the first 2 - 3 days after the onset of disease, and is present in urine and saliva for 2 to 3 weeks. Monkey kidney cells are generally used for virus isolation where a CPE is seen which consists of the formation of syncytia and the focal rounding of cells. Virus identification can be performed by neutralization or inhibition of haemadsorption by specific sera.
Syncytial formation caused by mumps virus. Note the presence of red blood cells on the surface of the cell sheet (haemadsorption). Courtesy of Linda Stannard, University of Cape Town, S.A.
F. Management and Prevention
No specific treatment is available for mumps. Uncomplicated parotitis seldom require treatment except adequate. Some authorities recommend a short course of corticosteriods in severe cases. Mumps is the commonest cause of meningitis and encephalitis in many countries such as USA and Scandinavia and many countries have mumps vaccination as part of their vaccination program. At one time, there was some argument as to whether a vaccination program against mumps was necessary but the combination of mumps with rubella and measles in the same vaccine had swung the argument vastly in its favour. An inactivated vaccine was first used in the 1940s successfully. This has now been replaced by a live attenuated vaccine. The protection rate is over 95% and no adverse reactions are associated with the vaccine. In the USA, where more than 40 million doses of mumps vaccine have been administered, a cost-benefit analysis has been carried out. In a cohort of 1 million people, the vaccine would prevent over 74,000 cases of mumps and 3 deaths and the cost-benefit ratio is 7.4:1. Mumps vaccine is now routinely given as part of the MMR regimen in many countries to all infants.